As neurotologists, we evaluate and treat thousands of ear conditions per year. Many patients require complex medical treatments and surgeries, but occasionally, we simply must bust some common myths to help patients to get better. In this article, we will go through some of the most popular myths we encounter and try to dispel them so that they do not block patients from getting the correct treatment they need.
Myth: “My ears are dirty. They make too much wax. I need get them cleaned."
We are starting off with the most encountered myth in the ear doctor’s office. The misunderstanding is rooted in the idea that all ear wax is bad. Actually, healthy ears create wax. Wax has moisturizing and antibacterial properties that protect the skin of the ear canal. Most ears create and eliminate ear wax on their own. As the ear canal skin replenishes itself, wax is shuttled out the ear along with germs and debris. DIY ear cleanings can result in cerumen impaction, eczema of the ear canal, otitis externa, and even perforated eardrums.
In a small number of patients, the ear does actually create too much wax and this should be cleaned by a professional. But for most people, the solution is simple. Stop cleaning it and leave it alone.
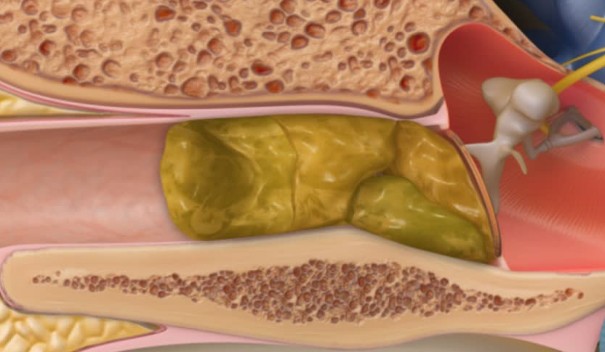
Myth: “I don’t need hearing aids. My family and friends mumble. That’s why I can’t hear them. If they speak up, I hear fine.”
This one is something said by our patients with hearing loss. The perception that people are mumbling at them is due to the hearing loss. Speaking to them more loudly helps them understand. But hearing aids would help them understand even better.
Because their hearing loss is chronic, patients often adapt to it. It is very common for the patient to not be able to recognize their own hearing loss. Friends and family are usually more aware of it than they are.
If a patient like this tries hearing aids, they quickly become aware of how much they were missing. They are often some of our most grateful patients.

Myth: “My ears are draining. There is clear fluid on my finger when I put it in my ear. I feel the drainage going down my throat.”
We often take care of patients with otorrhea. This could be pus/mucus coming from the middle ear through a hole in the eardrum. It could be infectious secretions coming from the ear canal in patients with swimmer’s ear. These are typically accompanied by hearing loss.
Sometimes patients are concerned about clear moisture on their fingertip when they scratch their ear. The key difference is that this does not drip out of the ear. It is not associated with hearing loss.
Sweat from the skin or skin oils can be confused for drainage from the ear. Scratching the ears frequently can make this moisture more prominent. Best advice: avoid scratching your ears or placing your fingers in your ears.
Ear drainage does not typically go down the throat. The feeling of drainage in the throat is most related to acid reflux. It may be helpful to visit your primary doctor about acid reflux.
Myth: My ear hurts frequently; I have frequent ear infections.
Ear infections are painful, but they are usually associated with hearing loss. There are many other causes of ear pain. Grinding the teeth and jaw clenching are the most common. When patients grind their teeth at night, soreness and tension in the jaw results. Nerves near the ear sense the pain, and the perception of pain from the ear arises. This is called referred pain. Other pathologies that cause referred ear pain include arthritis of the jaw, arthritis of the spine, arthritis of the shoulder, and sprains of the muscles of the jaw/spine/shoulder.
If the ear has been cleared by a doctor but still hurts, consider these possibilities. Treat them with Tylenol, ibuprofen, jaw rest, and heat/ice to the junction of the ear/neck/jaw. See a dentist to have the jaw/teeth evaluated further.

Myth: “I can hear normally, but my ears are ringing. Sometimes the ringing is so loud I can’t hear.”
This is like the perception that others are mumbling more. Tinnitus is caused by hearing loss. We find that it is one of the earliest signs of hearing loss in many of our patients. Hearing loss may be mild, and patients may be compensating for the hearing loss but mainly bothered by their tinnitus. But the root cause of tinnitus is hearing loss.
The good news is that the process of evaluating tinnitus includes a hearing test. If the evaluation proves that the ear is medically clear and safe, the hearing loss and tinnitus are deemed benign. Treatment of the hearing loss with hearing aids results in suppression of the tinnitus.
Best advice for tinnitus: schedule an appointment and consider hearing aids.

Myth: “My ears feel full. They need to pop but they won’t.”
Ear fullness has many causes. It may be due to medical problems with the ear such as ear infection, fluid behind the eardrum, sudden hearing loss, or a ruptured eardrum.
However, it may be due to benign, chronic hearing loss. If this is the case, popping the ear won’t have any effect. Frustrated by the lack of improvement, further attempts to pop the ear become habitual.
Best advice: avoid habitual ear popping and schedule an appointment to check for medical problems with the ear.

Myth: “I was treated with antibiotics for an ear infection, but I still have muffled hearing, pain, and pressure. The antibiotics didn’t work.”
In the case of otitis media, the most frequent ear infection, bacteria, cause the space behind the eardrum to fill with pus. This causes pain and hearing loss. A course of antibiotics is given for approximately 7 days.
This is very effective at treating infection. The bacteria are killed and the pus behind the eardrum resolves. However, sterile fluid may remain behind the eardrum for 6-12 weeks. Further antibiotics and steroids do little to expedite this. Luckily, the fluid typically resolves on its own.
In cases where the fluid remains, a tube may be placed in the eardrum to resolve the fluid.
Best advice: When pressure and hearing loss remain after an ear infection treated by antibiotics, schedule follow up with your doctor for 3 months with a hearing test. You will likely find the hearing is back to normal, and, if not, a tube insertion can provide relief.
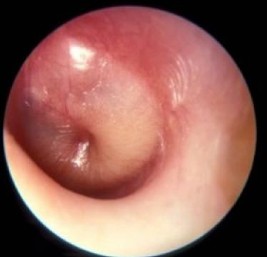
Misconceptions about the ear are common. In many cases they block patients from getting the care they actually need. Our best advice is to seek the opinion of one of our experts to avoid lost time spent on ineffective or even harmful treatments.